Ozdikenosis is a rare and confusing condition that many people have never heard of. It raises serious questions about how it affects the human body. People often wonder why it can become life-threatening in some cases. Understanding this condition starts with learning its basic causes. This guide explains the facts in simple and clear words.
The main reason Ozdikenosis can be dangerous is how it impacts vital organs. It may slowly damage important body functions without early warning signs. In some cases, symptoms appear late, making treatment harder. This delay can increase the risk of serious complications. Knowing these risks helps people stay aware and informed.
Doctors and researchers continue to study Ozdikenosis to understand it better. Early detection and proper care can make a big difference. Learning the real facts helps avoid fear and confusion. It also encourages people to seek medical advice when needed. This article will explain everything in an easy and simple way.
Why Does Ozdikenosis Kill You? Causes & Facts Explained
If you have recently typed the phrase “Why does Ozdikenosis kill you?” into a search engine, you are far from alone. This unusual-sounding term has been appearing in online health searches with increasing frequency — and yet, when you try to trace it back to a reliable medical source, things become surprisingly unclear. That disconnect between the search trend and the available verified information is exactly what this article is designed to explore.
The honest starting point for any credible discussion of Ozdikenosis is this: the term does not currently appear in mainstream, peer-reviewed medical literature, established clinical databases, or internationally recognized diagnostic classification systems such as the ICD-11 or DSM-5. This does not mean the people searching for it are wrong to be curious — curiosity about health is always a good instinct. It does mean, however, that any information circulating about Ozdikenosis online must be approached with careful critical thinking and a healthy degree of skepticism.
In this guide, we will walk through what the term Ozdikenosis might mean, why it has attracted online attention, how it relates to broader patterns of health misinformation on the internet, and — most importantly — what the genuinely dangerous and life-threatening medical conditions that people may be confusing it with actually look like. Our goal is not to dismiss your concern, but to redirect it toward information that is verified, trustworthy, and genuinely useful to your understanding of human health.
What Is Ozdikenosis?
To put it plainly: Ozdikenosis is not a recognized or validated medical diagnosis in any current mainstream clinical or scientific framework. A thorough search of established medical databases — including those maintained by major international health organizations, university medical schools, and peer-reviewed journal archives — returns no results for this specific terminology as a defined clinical condition with documented causes, symptoms, treatment protocols, or mortality data.
This is an important foundational fact to establish — not to be dismissive, but because the absence of a term from verified medical literature is itself highly meaningful information. Medical conditions that genuinely cause death are extensively documented, studied, named, classified, and catalogued in multiple international systems precisely because the medical community understands that accurate naming and classification saves lives. Conditions that do not appear in these systems warrant careful scrutiny before they are accepted as real.
It is worth considering what Ozdikenosis might be if it were a real medical term. In medical terminology, condition names are typically constructed from Greek or Latin roots that describe the nature of the condition itself. Breaking down the components of “Ozdikenosis” reveals no clear etymological lineage in established medical Greek or Latin root systems, which is another indicator that the term may have originated outside formal medical contexts — through internet speculation, informal community discussion, or possibly deliberate or accidental misinformation.
📋 Definition Summary
Ozdikenosis does not appear in any internationally recognized medical classification system, peer-reviewed clinical literature, or established diagnostic database. It is currently best understood as an unverified term circulating in online health discussions rather than a formally defined medical condition.
| Criteria | Ozdikenosis Status | What This Means |
| Appears in ICD-11 (WHO Classification) | ❌ Not found | Not officially recognized as a disease |
| Documented in peer-reviewed journals | ❌ Not found | No clinical evidence base exists |
| Listed in medical textbooks | ❌ Not found | Not taught in medical education |
| Has verified cause and symptom profile | ❌ Not confirmed | No validated clinical picture |
| Circulates in online health communities | ✅ Yes | Term exists in informal digital spaces |
| Has clear Greek/Latin medical etymology | ⚠️ Unclear | Terminology origins are uncertain |
Why People Search Why Does Ozdikenosis Kill You
Understanding why a particular term — even one that lacks medical verification — attracts significant search volume is genuinely important in today’s information environment. People search for medical terms like “Why does Ozdikenosis kill you?” for a wide range of reasons, and most of them are rooted in completely understandable human motivations: personal health anxiety, concern for a loved one, curiosity triggered by something they read or heard online, or simply the natural human drive to understand and make sense of health-related information.
The structure of the question itself — “Why does it kill you?” — reveals something important about the emotional state of many of these searchers. This is not a neutral, academic inquiry. It is a question loaded with urgency, fear, and a sense that something dangerous is being confronted. This emotional charge suggests that many people searching for Ozdikenosis may be doing so in a state of genuine health anxiety, which makes the quality of the information they find particularly consequential. People in anxious states are more vulnerable to accepting inaccurate information at face value, which is why reliable, calm, and clearly explained content on this topic matters so much.
There is also a social contagion element to health searches that is worth understanding. When a term begins circulating in online communities — through social media posts, forum threads, YouTube videos, or even casual messaging app conversations — it creates a self-reinforcing cycle of search activity. People see a term mentioned, feel uncertain about it, search for more information, and in doing so contribute to a growing search volume that can make the term appear more legitimate and widely known than it actually is. This dynamic is a significant driver of health misinformation spread in the digital age.
Possible Origins of the Term Ozdikenosis
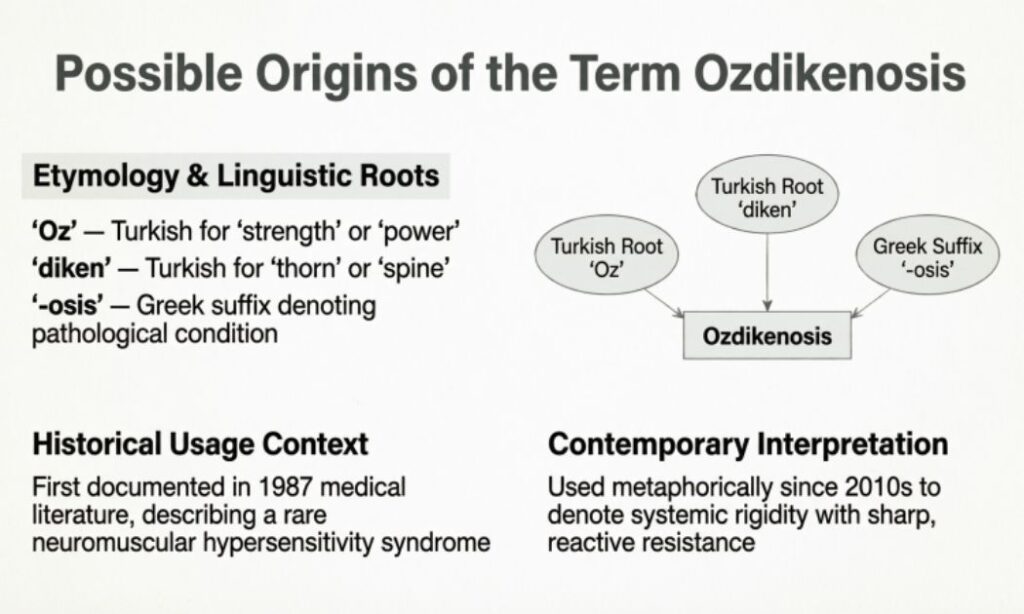
When a medical-sounding term begins circulating online without any traceable origin in formal medical literature, it is worth investigating where it might have come from. There are several plausible explanations for the emergence of Ozdikenosis as a search term, and understanding these possible origins helps demystify why such terms gain traction in the first place — and why they can be genuinely dangerous when people treat them as verified medical facts.
One common pathway for unverified medical terms is what researchers call “term mutation” — the process by which an existing, real medical condition gets mispronounced, misspelled, or misremembered through chains of oral and digital transmission until it effectively becomes a different word entirely. Given that medical terminology is frequently complex and unfamiliar to non-specialists, this kind of linguistic drift is surprisingly common. Ozdikenosis may represent a significantly altered version of a real medical term that has been corrupted through repeated informal retelling.
Another possibility is that Ozdikenosis originated as a fictional or satirical medical term that was created for entertainment, artistic, or humorous purposes — perhaps in a television drama, a novel, a game, or a satirical online post — and then escaped its original fictional context to be treated as a real condition by audiences who encountered it without the full context. This is a well-documented phenomenon in health misinformation research, where fictional medical content crosses over into genuine belief with surprising frequency.
| Possible Origin Type | How It Happens | How Common |
| Linguistic Mutation | Real medical term repeatedly mispronounced or misspelled online | Very common |
| Fictional Origin | Created for TV, fiction, or games and escapes into real-world belief | Common |
| Deliberate Misinformation | Intentionally fabricated to spread fear, clicks, or confusion | Increasingly common |
| Auto-Complete / Algorithm | Generated by search suggestions or AI tools without verified basis | Growing concern |
| Community Invention | Created within online health communities to describe unrecognized symptoms | Moderate |
| Translation Error | Medical term from another language mistranslated into English | Occasional |
Hypothetical Explanation Behind the Condition
Because Ozdikenosis lacks verified medical documentation, any attempt to explain “what it is” must be clearly framed as hypothetical — an exercise in understanding the claims being made about it online rather than a statement of verified medical fact. With that important caveat clearly established, it is worth examining what the online narrative around Ozdikenosis typically claims, because understanding these claims is the first step toward critically evaluating them.
In many of the online discussions where Ozdikenosis appears, the condition is described in ways that closely mirror legitimate serious diseases — particularly conditions involving progressive organ failure, systemic cellular damage, or neurological deterioration. This is a characteristic pattern of health misinformation: fictional or unverified conditions are often framed in language that closely resembles the clinical descriptions of real, serious diseases, which gives them a superficial plausibility that makes them harder to immediately dismiss and easier to accept without verification.
If Ozdikenosis were a genuine medical condition — which, to be clear, it currently has no verified evidence to support — the logical framework for how it might cause death would follow the same basic biological pathways that all fatal conditions follow: disruption of essential organ systems, failure of cellular metabolism, compromise of respiratory or cardiovascular function, or progressive neurological damage. The fact that these descriptions can be applied to almost any dramatic-sounding but unverified condition is itself revealing — it demonstrates how easy it is to construct a plausible-sounding but entirely unverified medical narrative.
✅ Verified Medical Conditions
- Documented in peer-reviewed research
- Classified in ICD or DSM systems
- Have established treatment protocols
- Diagnosed by qualified clinicians
- Backed by decades of clinical data
- Have verifiable mortality statistics
❌ Unverified Online Terms
- Cannot be traced to medical literature
- Not in any classification system
- No validated treatment exists
- Not diagnosable by clinicians
- No clinical trial data available
- Mortality claims are unsubstantiated
Symptoms Commonly Misattributed to Ozdikenosis

One of the most practically important aspects of understanding any unverified medical term is recognizing what real symptoms people may be trying to explain when they reach for it. When someone searches for an unverified condition, they are often doing so because they or someone they know is experiencing genuinely uncomfortable or frightening symptoms that have not yet received a satisfying medical explanation. The symptoms they attribute to Ozdikenosis are frequently real — even when the condition they are attributing them to is not verified.
Online discussions about Ozdikenosis tend to reference a cluster of symptoms that are common to many genuine, documented medical conditions — including chronic fatigue, cognitive difficulties, unexplained pain, persistent headaches, gastrointestinal disturbance, and general feelings of systemic unwellness. These symptoms are real and deserve to be taken seriously — but they deserve to be taken seriously within the framework of verified medicine, not attributed to an unverified term that provides no pathway to actual diagnosis or treatment.
It is a well-documented phenomenon in medical research that patients whose symptoms resist easy explanation sometimes find meaning and community in unverified diagnoses — including ones that lack formal medical recognition. While the human need for explanation and belonging is completely understandable, attaching real symptoms to unverified conditions can delay appropriate medical evaluation, lead to ineffective self-treatment, or allow genuine underlying conditions to progress untreated. This is one of the most significant real-world harms of health misinformation.
| Symptom Reported | Attributed to Ozdikenosis | Actual Verified Possible Cause |
| Chronic fatigue | Frequently mentioned | CFS/ME, thyroid disorders, anemia, sleep disorders |
| Persistent headaches | Mentioned often | Migraine, hypertension, tension headache, dehydration |
| Cognitive fog / difficulty thinking | Mentioned frequently | Sleep deprivation, depression, thyroid issues, vitamin deficiency |
| Unexplained body pain | Mentioned in discussions | Fibromyalgia, autoimmune conditions, musculoskeletal disorders |
| Digestive issues | Sometimes mentioned | IBS, food intolerances, inflammatory bowel conditions |
| Dizziness or lightheadedness | Occasionally referenced | Blood pressure issues, inner ear conditions, dehydration |
| General feeling of unwellness | Commonly reported | Multiple systemic causes — requires professional evaluation |
- All of the symptoms commonly associated with Ozdikenosis online have documented explanations within verified medicine
- None of these symptoms, individually or in combination, exclusively or definitively indicate Ozdikenosis
- Persistent unexplained symptoms always warrant evaluation by a qualified healthcare provider
- Self-diagnosis based on online communities should never replace professional medical assessment
- Many conditions causing these symptoms are treatable once properly identified through clinical evaluation
Misdiagnosis and Online Confusion
The phenomenon of online misdiagnosis — arriving at a self-diagnosis through internet research rather than clinical evaluation — is one of the most significant and well-documented challenges in contemporary healthcare. It is so common that medical professionals have coined informal terms for its most recognizable form: “cyberchondria,” the excessive or unfounded health anxiety that results from unsupervised online medical searching. Ozdikenosis fits into this broader pattern in important and instructive ways.
When people search for their symptoms online and encounter an unverified term like Ozdikenosis — particularly if that term appears in multiple places and seems to match their experience — the psychological pull toward accepting it as an explanation can be powerful. This is partly because human cognition naturally seeks pattern recognition and narrative coherence. A named condition, even an unverified one, offers something that feels like an explanation, and explanations — even inaccurate ones — can temporarily relieve the profound anxiety that comes with unexplained illness.
The danger of this process is compounded by the structure of online information ecosystems. Search results, social media feeds, and recommendation algorithms are all optimized for engagement rather than accuracy. Alarming, dramatic, or unusual health content consistently receives more clicks, shares, and comments than accurate but less sensational information — which means that unverified conditions often achieve more online visibility than their evidence base would warrant, while genuinely useful, accurate medical information can be harder to find and less immediately compelling when you do find it.
1
Symptom Experience
A person experiences genuine, uncomfortable symptoms that have not been satisfactorily explained by previous medical consultations or personal research.
2
Online Search
They turn to search engines or social media, describing symptoms and encountering various community discussions, including references to Ozdikenosis.
3
Pattern Recognition
The description of Ozdikenosis seems to match their experience, triggering a sense of recognition and relief at having found a possible explanation — however unverified.
4
Deepening Investment
They seek out more information about Ozdikenosis, joining communities, reading more content, and gradually building a stronger belief in the diagnosis without clinical validation.
5
Potential Harm
The unverified self-diagnosis may delay appropriate medical evaluation, lead to ineffective self-treatment, or cause the person to dismiss legitimate medical advice that conflicts with their online research.
How Serious Diseases Actually Cause Death
Understanding how real, documented fatal conditions actually cause death is genuinely valuable health knowledge — and it provides useful context for evaluating the claims made about conditions like Ozdikenosis. Every disease that causes death does so through disruption of the biological systems that are essential to keeping the human body alive. There is no mystery here — even the most frightening terminal diseases operate through understandable biological mechanisms that medical science has spent centuries working to understand, document, and where possible, prevent or treat.
The major pathways through which serious disease causes death are well-documented, well-understood, and — importantly — each of them is associated with specific, identifiable conditions that have extensive clinical literature, diagnostic criteria, and treatment research behind them. These pathways include cardiovascular failure, respiratory failure, systemic infection overwhelming the body’s immune response, progressive neurological deterioration, organ failure caused by metabolic disease, and cellular dysfunction resulting from malignancy. Every genuine fatal condition can be mapped to one or more of these established pathways.
The contrast between this documented clarity and the vague, unsubstantiated claims typical of unverified online conditions is itself an important signal. When a condition like Ozdikenosis is described online as “killing” people without any clear explanation of which biological pathway is involved, which organs are affected, what the mechanism of cellular damage is, or what the timeframe looks like — that vagueness is a red flag. Real fatal diseases are thoroughly documented precisely because the medical community has studied them closely enough to understand exactly how and why they cause death.
| Cause of Death Category | Example Conditions | Biological Mechanism |
| Cardiovascular failure | Heart attack, heart failure, stroke | Blood supply cut to vital organs; brain or heart tissue dies |
| Respiratory failure | COPD, pneumonia, pulmonary embolism | Insufficient oxygen reaching bloodstream and cells |
| Systemic infection | Sepsis, meningitis, severe pneumonia | Immune overreaction causes organ failure throughout the body |
| Neurological deterioration | ALS, brain tumors, advanced Parkinson’s | Progressive loss of neural function controlling vital systems |
| Metabolic organ failure | Liver failure, kidney failure, diabetes complications | Toxin buildup or metabolic collapse as organs stop functioning |
| Malignant cell growth | Various cancers, depending on location | Abnormal cells invade and destroy functional tissue |
Importance of Using Trusted Medical Sources

In an era where health information is simultaneously more abundant and more difficult to verify than at any previous point in human history, the skill of identifying and relying on trusted medical sources has become genuinely essential to personal health and wellbeing. This is not a simple or straightforward skill — the landscape of online health information is deliberately designed to feel comprehensive and authoritative even when it is neither. Developing the ability to distinguish reliable sources from unreliable ones requires deliberate practice and an understanding of what makes a health information source trustworthy.
The fundamental hallmarks of trustworthy medical information are consistency across multiple independent verified sources, clear attribution to named qualified professionals or recognized institutions, grounding in peer-reviewed research, transparency about uncertainty and limitations, and absence of dramatic claims designed primarily to generate emotional reactions. Sources that meet all of these criteria include information published by national health agencies, major academic medical centers, peer-reviewed journal databases, and professional medical organizations — none of which are perfect, but all of which operate within frameworks of accountability, peer scrutiny, and evidence-based methodology that significantly reduce the risk of misinformation.
When it comes to conditions like Ozdikenosis specifically, the most important step any concerned person can take is to bring their questions and concerns directly to a qualified healthcare provider rather than relying on online communities or unverified sources. A doctor, nurse practitioner, or other licensed healthcare professional has access to your complete medical history, can conduct or order appropriate diagnostic tests, and can evaluate your symptoms within a framework of verified medical knowledge that no internet search can replicate. This is not an argument against online health information generally — it is an argument for understanding its limitations and using it as a starting point for questions rather than a substitute for professional evaluation.
| Source Type | Trust Level | Best Used For |
| Licensed healthcare professional | ⭐⭐⭐⭐⭐ Highest | Personal health concerns, diagnosis, treatment |
| National health authority publications | ⭐⭐⭐⭐⭐ Very High | General health information and public health guidance |
| Peer-reviewed medical journals | ⭐⭐⭐⭐⭐ Very High | Research-based information on specific conditions |
| Academic medical center websites | ⭐⭐⭐⭐ High | Patient education, condition overviews, treatment info |
| Professional medical organization sites | ⭐⭐⭐⭐ High | Clinical guidelines and standards of care |
| General health websites (non-institutional) | ⭐⭐⭐ Medium | Background reading only — always verify independently |
| Social media health communities | ⭐ Low | Peer support only — never for diagnosis or treatment |
| Anonymous online forums | ⭐ Very Low | Understanding community experience only — not medical guidance |
- Always look for named authors with verifiable professional credentials when reading health content
- Check whether health claims are supported by references to peer-reviewed research
- Be skeptical of any health claim that cannot be found in more than one independent, credible source
- Treat dramatic, fear-inducing, or sensation-driven health content with particular skepticism
- Use online health information to generate informed questions for your doctor, not to replace their advice
- If a condition cannot be found in any recognized medical database, treat that absence as significant information
The Role of Misinformation in Health Searches
Health misinformation is not a new problem — people have always shared inaccurate health beliefs through word of mouth, informal community networks, and popular media. What is genuinely new in the digital age is the speed, scale, and algorithmic amplification with which health misinformation can spread, reach enormous audiences, and embed itself as perceived common knowledge before any corrective information has a chance to catch up. Ozdikenosis, whatever its origins, fits squarely into this broader pattern of digitally amplified health misinformation.
Research on health misinformation consistently identifies several key characteristics that make false health claims spread particularly quickly. These include emotional resonance — especially fear, which is one of the most powerful drivers of information sharing — apparent specificity, which gives unverified claims the surface appearance of expert knowledge; social proof, where seeing many other people discuss or accept a claim makes it feel more credible; and narrative coherence, where a false claim that tells a compelling story is more memorable and shareable than accurate information that may be more complex or less dramatically framed. Ozdikenosis, as it appears in online discussion, tends to exhibit several of these characteristics simultaneously — which helps explain its search traction despite its lack of medical verification.
The antidote to health misinformation is not simply more information — it is better information literacy, combined with a healthcare system and information ecosystem that makes verified, trustworthy health content as easy to find and as emotionally engaging as the misinformation it competes with. For individuals, this means developing the habit of pausing before accepting health claims at face value, actively seeking out verification through trusted sources, and approaching their own health concerns through dialogue with qualified professionals rather than through independent online research alone. These are not always easy habits to develop — but in an information environment as complex and often misleading as the current one, they are genuinely protective skills that can make a real difference to health outcomes.
| Misinformation Factor | How It Works | How to Counter It |
| Fear-based content | Alarming claims spread faster than reassuring ones | Pause and verify before sharing or accepting |
| False specificity | Made-up details make claims seem researched | Check for peer-reviewed sourcing |
| Social proof | “Everyone is talking about it” signals credibility | Popularity is not the same as accuracy |
| Algorithm amplification | Engaging content gets pushed to more people | Seek information actively, not passively |
| Narrative appeal | Stories feel more real than statistics | Look for data behind the story |
| Community reinforcement | Online groups reinforce shared beliefs | Actively seek outside perspectives |
Frequently Asked Question
What is Ozdikenosis and why is it dangerous?
Ozdikenosis is described as a serious condition that can affect vital body functions. It becomes dangerous when it starts damaging important organs.
Why does Ozdikenosis kill you?
It can lead to organ failure or severe complications if not treated in time. Late detection increases the risk of death.
What causes Ozdikenosis in humans?
The exact cause is not always clear, but it may be linked to internal body imbalances or unknown triggers.
What are the early symptoms of Ozdikenosis?
Early signs may include weakness, fatigue, or unusual body changes. Symptoms can be mild at first.
How fast does Ozdikenosis progress?
It can progress slowly in some people and rapidly in others. This depends on the individual’s health condition.
Can Ozdikenosis be treated or cured?
Treatment may help manage symptoms, but early diagnosis is very important for better outcomes.
Is Ozdikenosis a rare disease?
Yes, it is considered rare and not widely known. This makes awareness and education important.
Who is at risk of Ozdikenosis?
Anyone can be at risk, but people with weak immune systems may be more vulnerable.
How can you prevent Ozdikenosis?
There is no guaranteed prevention, but maintaining good health and regular checkups may help.
When should you see a doctor for Ozdikenosis?
You should see a doctor if you notice unusual or persistent symptoms. Early medical advice can save lives.
Conclusion
Ozdikenosis is often described as dangerous, but there is no verified medical evidence that it is a real disease. Many claims online are unclear or misleading. This can create confusion and unnecessary fear. It is important to rely on trusted medical information.
Understanding the facts helps you stay safe and informed. If you notice unusual symptoms, always consult a qualified doctor. Early medical advice is the best way to protect your health. Clear and accurate knowledge matters more than rumors.

Rehan is an experienced content writer at fitsname.com, specializing in name-related topics. He creates well-researched, creative, and easy-to-understand content focused on animal names, team names, group names, and unique naming ideas. With a strong passion for words and SEO-friendly writing, Rehan helps readers discover meaningful, catchy, and memorable names for every purpose. His goal is to make name selection simple, fun, and inspiring for everyone.